Revolutionising research with innovative clinical trials

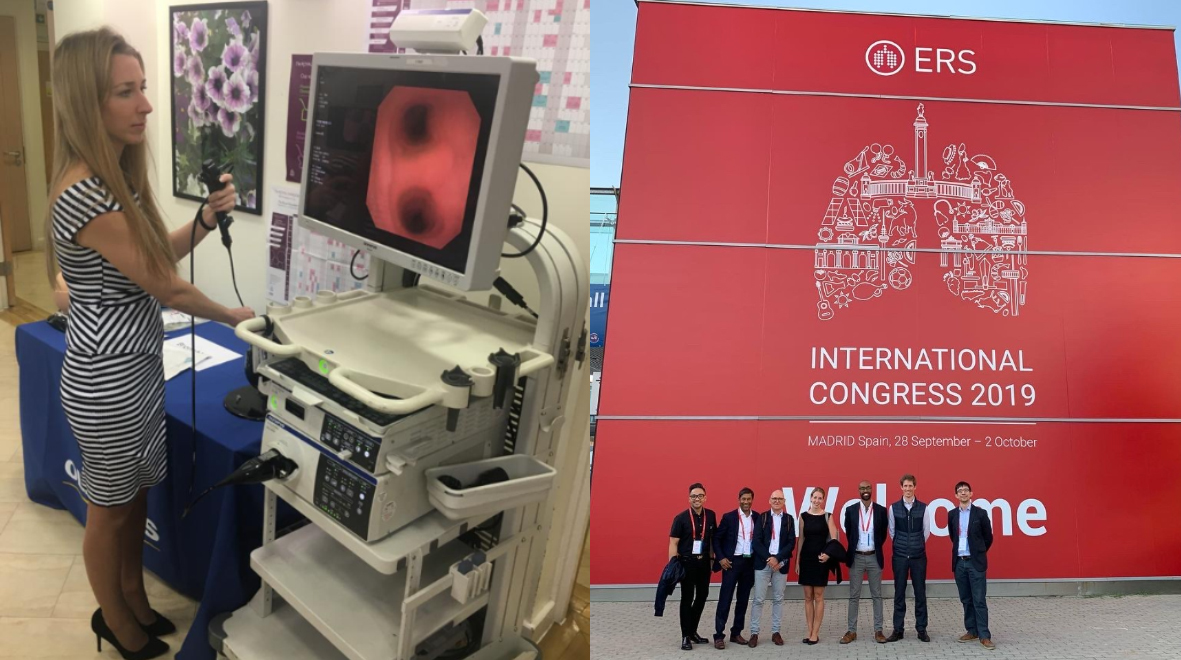
On Clinical Trials Day, Prof Otavio Berwanger, Executive Director of The George Institute for Global Health and Chair in Clinical Trials at Imperial College London, shares how rethinking the design and delivery of clinical trials can benefit all involved in medical research.
Large-scale and high-quality randomised controlled trials (RCTs) are considered the gold standard in clinical research. Study participants are randomly allocated to intervention or control groups and their outcomes are compared, minimising bias and providing reliable evidence about the efficacy and safety of treatments. Clinical trials have been vital to some of the biggest advances in modern medicine, but they are not without their drawbacks.
Conducting RCTs is an expensive, time-consuming, and complex process. They take several years to complete and cost millions of pounds;. Participants are also required to travel to central trial sites for assessments, making patient recruitment and participation difficult.
In response to these challenges, we have formed the Innovative Clinical Trials Hub. The hub aims to support projects across The George Institute, Imperial and those led by external organisations, to design, deliver and analyse innovative, efficient, and impactful, large-scale, patient-centric trials. In this sense, we are very proud of our excellent partnership with the Imperial Clinical Trials Unit (ICTU) and we will definitely work together in delivering high-quality, innovative trials. Similarly, we see great opportunities for developing efficient trial models in other regions, including Australia (where we have a strong partnership with the University of New South Wales -UNSW) and India. I am also very excited to collaborate with the UKCRC Clinical Trial Units network in my capacity as the new Chair of the International Registration Review Committee.


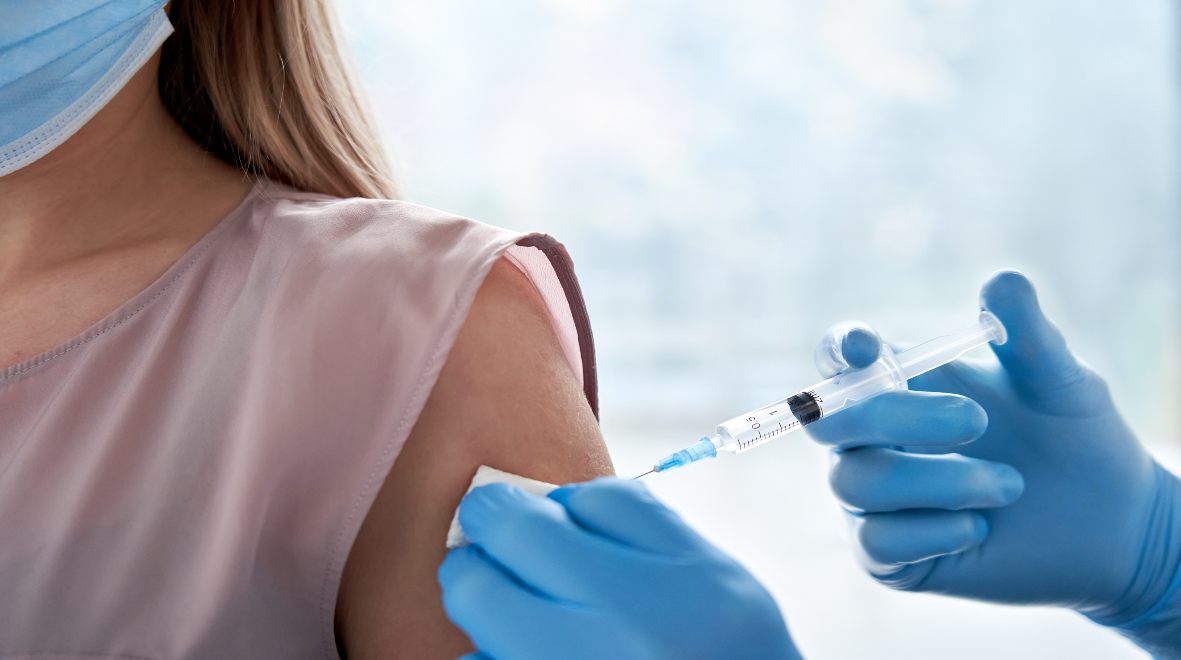
 How do you engage members of the public with medical research? Dr Emma Smith, HIC-Vac Network Manager, outlines how consulting the public was crucial during the world’s first COVID-19 human challenge study.
How do you engage members of the public with medical research? Dr Emma Smith, HIC-Vac Network Manager, outlines how consulting the public was crucial during the world’s first COVID-19 human challenge study.