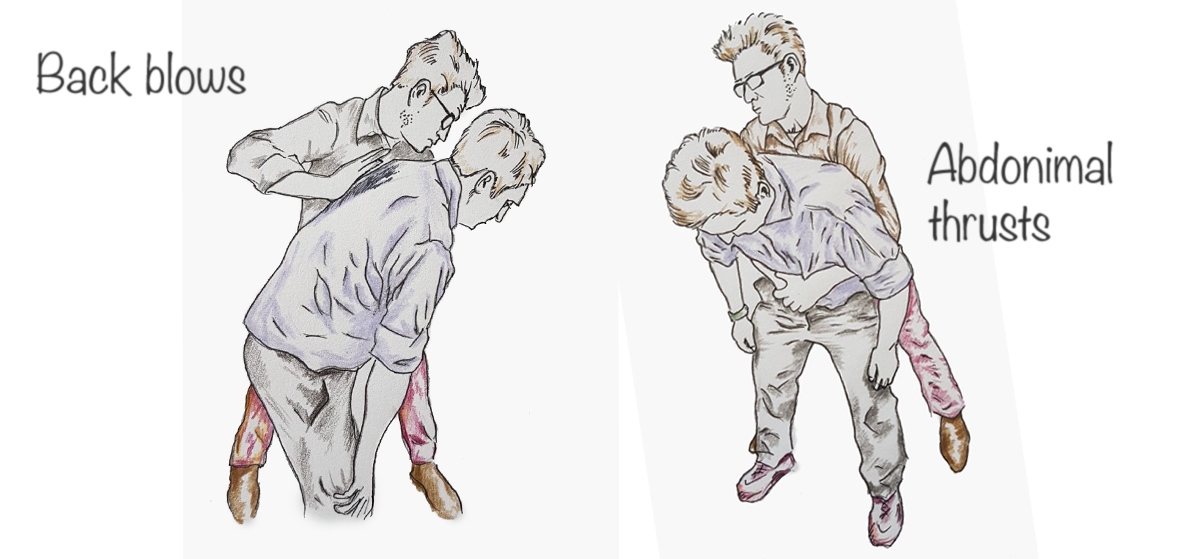
Can we trust the tobacco industry?

Originally published on Dr Nick Hopkinson’s blog and reproduced here with permission, this post looks at the Tobacco Industry’s dark history of appropriation and subversion of science.
“It ain’t no new thing” sang Gil Scott Heron in 1972, condemning the appropriation of black culture by white recording artists. A recent research paper published in Tobacco Control throws light on Tobacco Industry appropriation and subversion of science. Their goal, to prevent or delay measures which reduce their ability to market products that are among the leading causes of death worldwide (1). (more…)